Blog
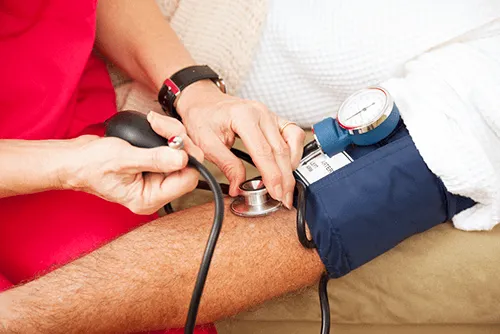
15 Things to Know About Medicare and home care
If your loved one is covered by Medicare and needs home care, there are certain guidelines you need to follow to ensure they get the care they require. Medicare and home care agencies work closely together to create a care plan for patients, but there are things you need to know about that partnership.
15 Things to Know About Medicare and home care
You Must Be Under the Care of a Doctor
You aren’t able to just contact a home care agency and arrange for a caregiver to visit your house. You must be under the care of a physician who has determined that home care is a necessity to help you recover from an injury or illness. A care plan between the doctor and the home care agency must be established and reviewed by the doctor on a regular basis to assess your progress.
You Must Be in Need of Specific Medical Services
You can only receive home care services if your doctor determines you need one or more of the following medical services.
- Physical therapy
- Continued occupational therapy
- Speech-language pathology services
- Intermittent skilled nursing (except blood draws)
- Injectable osteoporosis drugs for women
- Intermittent personal hands-on care
- Medical social services
Intermittent Skilled Nursing
Examples of intermittent skilled nursing services that would be covered by Medicare include wound care, catheter care, intravenous (IV) therapy, vital signs monitoring, tube feeding, application of dressings that involve prescription medications, heat treatments, administration of medical gases, supervision of toileting, nutrition education, caregiver and patient education, and more.
Intermittent care is defined as skilled nursing services you receive fewer than seven days a week or for fewer than eight hours a day over a 21-day period. In some cases, more frequent care may be approved, but your doctor will need to submit evidence to Medicare that more care is medically necessary for your condition. Without this approval, you may be responsible for some out-of-pocket charges.
Intermittent Personal Hands-On Care
A home health aide (rather than a registered nurse) is able to perform personal hands-on care services to you through Medicare. Examples of services that fall under the personal hands-on care category include help with daily tasks like dressing and bathing, assistance with household tasks like cooking and cleaning, and various other non-medical services.
Medical Social Services
Medical social services are those that are necessary for patients and family members who are coping with an advanced illness. They may include assessing the emotional factors related to the illness, evaluating the patient’s living situation, evaluating the patient’s financial resources, and assessing the availability of community support to aid in recovery. Counseling may also be provided to the patient and their loved ones.
Medicare Must Approve the home care Agency
The home care agency you use to provide services in your home must be approved by Medicare. There is a list maintained on the Centers for Medicare and Medicaid Services (CMS) website that can provide you with a full list of Medicare-approved agencies in your area, but you can also get recommendations from your physician or your State Survey Agency.
You Must Be Homebound
To be eligible to receive home care services through Medicare, you must be certified as homebound by your doctor. This means that due to an injury or illness, you cannot leave your home without the help of a wheelchair, crutches, a cane, a walker, special transportation, or assistance from another person. You may also be certified as homebound if the doctor doesn’t recommend leaving your home because of your illness or injury, even if you are physically able to.
You Must Have a Face-to-Face Encounter With a Doctor
You are required to actually see the doctor or a healthcare professional who works with the doctor who recommends home care. This means the doctor cannot determine that home care is warranted by just speaking with you or a family member over the phone. While telehealth is considered an acceptable substitution for face-to-face encounters during the COVID-19 crisis, Medicare still may require an in-person visit.
Medicare Covers Home Health Services at 100%
As long as you meet all the requirements for home care services, including being certified homebound, Medicare will cover the services at 100%. You will pay nothing out-of-pocket for approved home care services such as those mentioned above. If you require any durable medical equipment as part of your care plan, it will be covered at 80%, meaning you will be responsible for 20% of the covered amount.
You Can Choose Your home care Agency
If you already have a home care agency in mind that you want to use for your home care services, your choice should be honored by your physician, as long as the agency is certified by Medicare. For this reason, you and your loved ones should carefully research the agencies near you to ensure they offer the services you need and that their quality ratings are high. It’s also beneficial to get patient references for any agency you consider.
Certain home care Services Are Not Covered by Medicare
While most medical services delivered by a nurse and personal hands-on care services delivered by a home health aide are covered by Medicare, there are some services that are excluded from Medicare’s coverage. These include the following services.
- Meal delivery
- Round the clock care
- Homemaker services when they are the only services you need
- Personal care services when they are the only services you need
Homemaker services include shopping, cooking, and cleaning and personal care services include bathing, dressing, and toileting. Many of these services are covered by Medicare if they are necessary due to the limitations of your injury and illnesses. To ensure they are covered, you’ll want to ask your doctor to include them in your care plan. The need for these services will be consistently re-evaluated by your doctor as you recover from your injury or illness.
There Are Additional Criteria for Home Health Physical and Occupational Therapy
To qualify for home health physical and occupational therapy you have to meet one of three additional criteria: your condition must be expected to improve over a reasonable amount of time, or you require the services of a skilled therapist to develop a maintenance program for your condition in a safe and effective manner, or you require the services of a skilled therapist to do maintenance therapy for your condition in a safe and effective manner.
Your Care Plan Should Include Your Input
Although a care plan is mostly developed through a collaboration between your doctor and your home care agency, your input is valuable and should be included in the plan. When the home care agency meets with you to set up your care, explain what your goals are for getting home care, how long you intend to need it, and the services you expect to receive. You may be eligible for services your doctor didn’t consider at first.
When you’ve suffered an injury or illness, it can be difficult to get the care you need if you have to travel to a facility each time you need it. Fortunately, Medicare covers home care and can help you receive proper nursing and personal care as you recover from your injury or illness. Contact Parent Care to see how our healthcare professionals can make your life easier and healthier.